Authors
Kalina Sanders , Neurologist & Samantha Balistreri , Physical Therapist
Close

4 Jan 2026 | ~03:22 Engagement Time
For decades, MS was grouped into familiar categories: relapsing-remitting MS (RRMS), primary progressive MS (PPMS), secondary progressive MS (SPMS), and sometimes clinically isolated syndrome (CIS). These labels helped clinicians describe the overall type of MS someone had and were important for diagnosis, treatment decisions, insurance, and long-term tracking.
But over the years, people living with MS have shared something important:
Clinicians and researchers have heard you.
Across MS centers, academic research, and community programs, the field is shifting toward a more dynamic, real-time way of describing MS—one that blends the biology of inflammation and progression with your lived experience. The shift better recognizes that MS is not a static condition. Your disease course can—and often does—change over time.
The traditional categories (RRMS, PPMS, SPMS, CIS) are no longer viewed as the best way to understand what MS is doing right now.
Here’s what’s happening across the MS community:
Instead of relying only on the old labels, experts now ask two key questions to understand your MS in real time:
These three dimensions—activity, worsening, and progression—combine to paint a much fuller and more accurate picture of how MS is affecting you right now, not just what your MRI shows or which category you were assigned years ago.
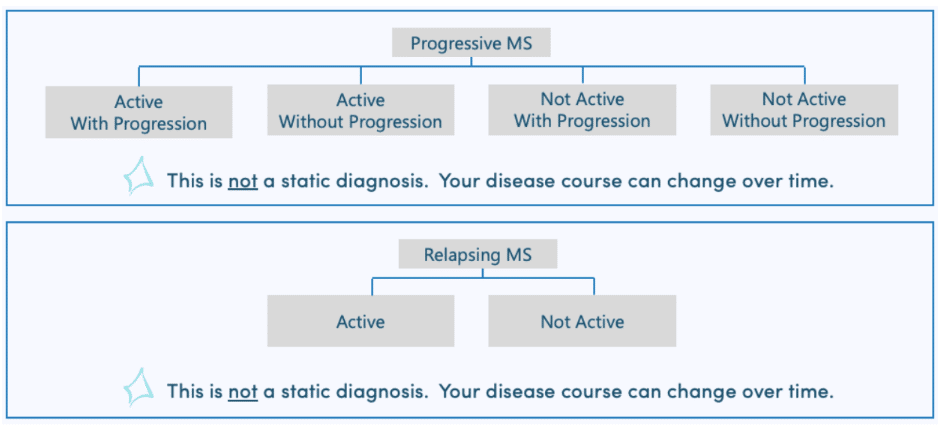
The MS field is in a period of transformation. You may hear both old and new terminology for years to come. What’s most important is:
Our goal in this series is to discuss the different MS disease courses and to help you bridge the gap between older categories and this more personalized, evolving view of MS.
Keep Learning...