About COVID-19
COVID-19, or “coronavirus disease of 2019”, is the disease caused by the virus, SARS-CoV-2. There are many different coronaviruses and some of them cause illness in animals and people. SARS-CoV-2 stands for “severe acute respiratory syndrome coronavirus 2”. MS does not increase your risk for getting COVID-19.
When did COVID-19 first appear in people?
The first case of COVID-19 was reported Dec. 1, 2019. This new virus, which had never previously been seen in humans, was soon named SARS-CoV-2. SARS-CoV-2 may have originated in an animal and changed (mutated) so it could cause illness in humans. SARS-CoV-2 spread rapidly. By March 11, 2020, the World Health Organization (WHO) officially labeled the COVID-19 outbreak a worldwide pandemic. This designation meant that the virus had spread to people over several countries or continents and had infected many people.
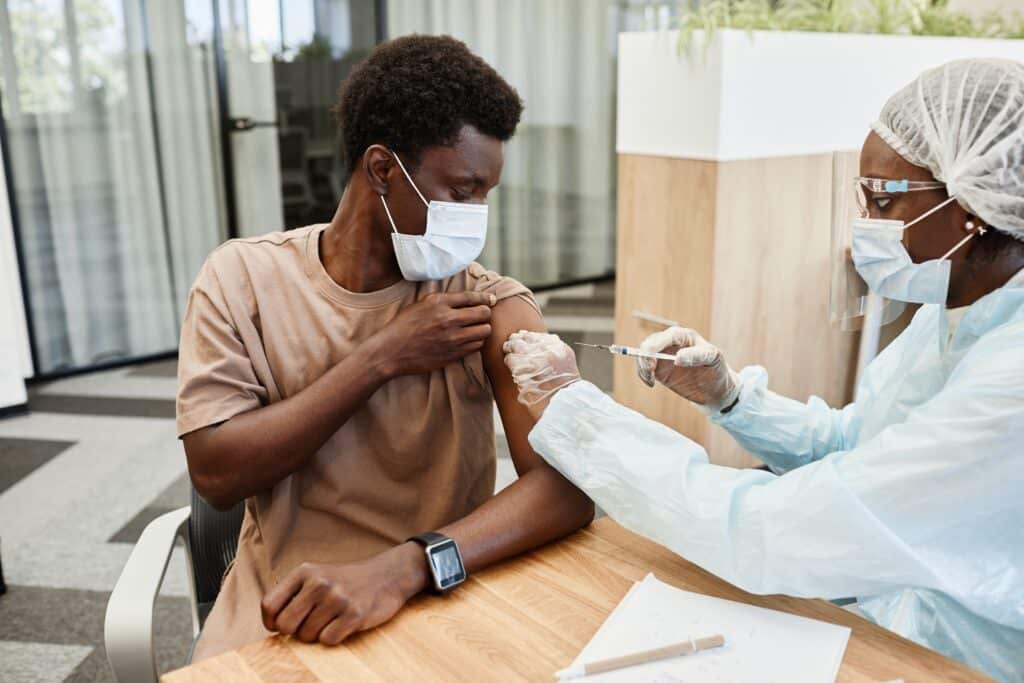
How does the virus spread?
The virus that causes COVID-19, SARS-CoV-2, is spread by respiratory “droplets” and that means that it is transmitted from the respiratory system to another person by a cough, sneeze, or even by just breathing normally near another person.
What are SARS-CoV-2 variants?
Over time, viruses can change, or mutate, meaning that the physical structure of the virus can evolve and adapt as needed for the virus to survive. Often these structural changes can make the virus more transmissible from one person to another, or able to cause milder or more severe illness. Virus mutations also mean that the virus may be able to avoid immunity from a vaccine or from previous infection. This does not mean that people should abandon COVID-19 vaccination, as research has shown that vaccination reduces the risk of severe illness or death.

Symptoms
Symptoms vary and for many, it may feel like a common cold. For others it may feel like the flu and for some it will make them sick enough to know they need a hospital visit. Typical symptoms may include:
- Fever
- Chills
- Shortness of breath or difficulty breathing
- Cough
- Runny nose
- Sore throat
- Loss of sense of taste and/or smell
- Joint aches
- Muscle pain
- Headache
- Nausea/vomiting
- Diarrhea
COVID-19 and MS
Having MS does not make you more susceptible to getting COVID-19. The National MS Society identifies the following characteristics as associated with more severe infection:
- Progressive MS
- Older age
- Male sex
- Black race
- Mobility issues that require a mobility device or a wheelchair
- Obesity
- Other chronic health problems – diabetes, heart disease – in addition to MS
- Taking steroid medications (such as prednisone, methylprednisolone, dexamethasone, and others)
- Taking certain MS disease modifying treatments (including drugs such as rituximab and ocrelizumab)
What is long COVID?
Long COVID consists of symptoms that persist after the initial infection with SARS-CoV-2 has cleared. These symptoms can last for weeks, months and even years. Having MS does not make you more susceptible to long COVID. Symptoms of long COVID may include one or more of the following:
- Severe fatigue
- Cough
- Shortness of breath
- Headaches
- Joint pain
- Difficulty thinking – often called “brain fog”
- Stomach pain
Brain Fog: A slow, fogginess in your thinking.
Is this something you struggle with? Read 12 Tips For Brain Fog for some solutions.
What is the effect of MS medications COVID-19 risk and vaccine response?
MS medications and infection
Certain medications taken for your MS may increase the risk of more severe COVID-19.
MS medications that modify the MS disease process have an effect on the body’s immune system. Some of these medications, including anti-CD20 medications (such as Ocrevus® and Rituxan®) may increase the risk for a more severe case of COVID-19 – meaning a greater likelihood of needing hospitalization or breathing support.
Other medications that work similarly may also increase risk of more severe COVID (Kisimpta® and Briumvi®, but less is known about their risk at this time.

MS medications and COVID vaccines
Certain MS DMT’s also reduce the immune response to COVID vaccines. These include the anti-CD20 drugs noted above and also S1P receptor modulators like Gilenya®. This does not mean you should avoid the COVID vaccine, but it does mean that the timing of the vaccine is important to your immune response.
Please see the National MS Society COVID-19 guidance for further information about MS medications and COVID-19. Consider speaking with your MS provider about MS and COVID-19 and the timing of COVID vaccination.

Infection Prevention
The SARS-CoV-2 virus and COVID-19 will be with us for the foreseeable future. Here are a few proven strategies that can reduce your risk of becoming infected with SARS-CoV-2:
- Get vaccination and boosters for SARS-CoV-2. Follow specific National MS Society COVID-19 vaccine guidance if you are on an MS disease modifying treatment
- Wear a mask when in malls, churches, stores, indoor gatherings, and other places where there are groups of people
- Keep physical distance (about 6 feet) between yourself and others
- Wash your hands frequently and thoroughly
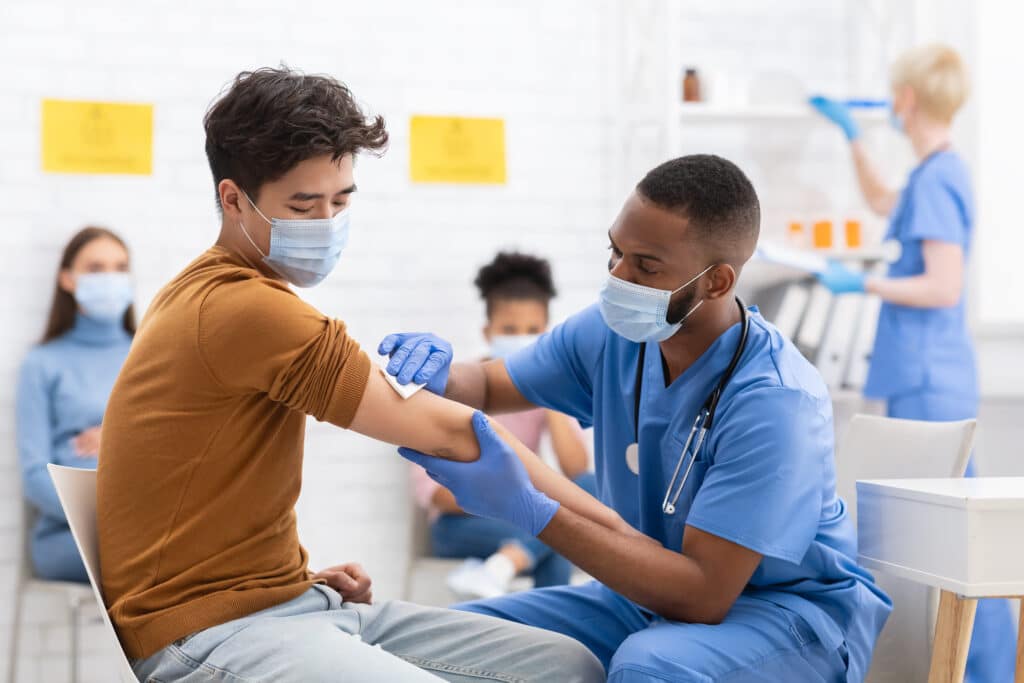
More About COVID and MS
Useful Links
